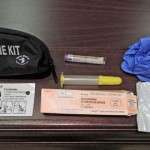
Photo by Phil Eil
by: Phil Eil • 630WPRO.COM
Rhode Island is in the midst of an epidemic.
According to the most recent Department of Health numbers, there have been 212 apparent accidental drug overdose deaths in 2014, in 31 cities and towns, involving “men and women of all ages and ethnicities.”Those numbers bear repeating: 212 deaths, in 31 (of 39) cities and town. And according to RIDOH, “Of the total number of apparent accidental drug overdose deaths since January 1, 2014, 187 (90%) of the screened cases involved at least one opioid or medication.”
Now, we could – and should – have a much larger conversation about why this situation hasn’t triggered the same kind of sirens-blaring, spinning-red-lights alert as, say, 212 Rhode Islanders dying from ebola or the EEE virus. But let’s save that for another day. For now, it’s worth highlighting a reason why those terrifying, heartbreaking numbers aren’t even higher: naloxone.
Naloxone, the opioid reversal agent sold under the brand name “Narcan,” isn’t anything new. Hospitals have been using it for decades to control the effects of opioid medications (narcotic pain relievers like OxyContin, Vicodin, and Percocet) administered to patients. But in the last 12 months, the medication has become more accessible in the Ocean State than ever before.
One might say it’s your civic duty to learn more about it.
WHAT IS NARCAN?
Naloxone works powerfully and near-instantaneously when placed under a patient’s tongue, sprayed into their nose, or injected into an arm or leg. And if it’s administered soon enough after a patient shows the signs of an opiate overdose (blue lips, shallow breathing, general non-responsiveness), the patient can “wake up” almost as if nothing has happened. People who have seen the drug work often refer to it as “magic,” or a “miracle drug.”
“I think the easiest way to think of it is, it’s the opposite of an opiate,” says Dr. Jim McDonald, Chief Administrative Officer on the Board of Medical Licensure and Discipline at the RIDOH. “It blocks where the medicine would get into our body, and it makes the medicine like it’s not there at all.”
“It goes to the opioid receptors in the brain,” says Miriam Hospital researcher and senior project director, Michelle McKenzie. “And when there are opioids in the receptors, which is what is happening when a person is overdosing from opioids, the Narcan literally goes into those receptors and binds them really strongly and kicks out the other opioids.”
It’s worth noting that though a Narcan-revived overdose victim may appear “fine,” the person is still in danger. Jared Moffat, a volunteer instructor with Preventing Overdose and Naloxone Intervention (PONI) explains that the medication wears off after anywhere between 30 and 90 minutes. “So once it wears off, the opioids, if they’re still in the bloodstream, can re-bind to those receptors,” he says. “But it gives at least a temporary window in which someone can come out of the overdose and be treated.”
“It is tremendously effective,” says Brown University Professor of Medicine and Epidemiology, Dr. Josiah Rich, who credits Dan Bigg, the founder and co-director of the Chicago Recovery Alliance, with bringing the medication out of hospitals and into the hands of public health workers and everyday citizens. The change in policy followed the heroin OD death of one of CRA’s founders, Bigg has explained to harmreduction.org. “In the fall of 1996, after sadness turned to desire for action, myself and some MD friends started naloxone training and distribution to select CRA participants,” he said. “In January 2001, CRA rolled out its first OD training for all staff and interested volunteers and participants and incorporated naloxone distribution to all sites and contact points CRA operates. At this time, we also posted materials on our website for any other program to use. Through spreading the word through the Harm Reduction community about the effectiveness of naloxone distribution, by the late 1990s and early 2000s other programs in the US began to start distributing naloxone.”
Since then, naloxone has become increasingly available to public health workers, drug users, and their families and friends. It’s also caught on with law enforcement agencies that see it as a critical way for officers – often among the first to arrive at the scene of an overdose – to “serve and protect” their communities. The Quincy, Massachusetts Police Department has been a national leader in the implementation of Narcan. In October, the QPD reported its 300th successful use since January 2011.
2014: YEAR OF NARCAN
2014 has been a marquee year for naloxone/Narcan.
In February, after the heroin overdose death of Philip Seymour Hoffman, the New York Times published an op-ed, “How to Stop Heroin Deaths,” by an ER physician who wrote that the actor “was just one of hundreds of New Yorkers who fall victim to this drug each year.”
“The most frustrating part is that each of these deaths is preventable, because there is an antidote to heroin overdose that is nearly universally effective,” he continued. “Naloxone, an opioid antidote, is a simple compound that has been in clinical use for more than 30 years.”
In July, US Attorney General Eric Holder issued a memo urging federal law enforcement agencies to train and equip officers who may come in contact with heroin OD victims. “I am confident that expanding the availability of naloxone has the potential to save lives, families and futures of countless people across the nation,” Holder said in a press release reporting over 100 Americans die every day from drug overdoses, which is more than gunshot deaths or traffic accidents.
And earlier this month, VICE News released a 15-minute documentary, “Back from the Brink: Heroin’s Antidote,” chronicling Narcan’s use in Quincy and other towns across Massachusetts.
Rhode Island hasn’t garnered quite as much attention as our Northern neighbor. But we still have a lot to be proud of. In March, the Department of Health Issued new emergency regulations aimed at “Expanding Use of Narcan to Prevent Opioid Overdose Deaths.” In May, the Rhode Island State Police announced it had trained its force to administer Narcan and distributed over 175 kits to patrol troopers and detectives. (Weeks later, a trooper administered Narcan during a traffic stop in Hopkinton, stabilizing the man’s breathing until an ambulance arrived.) In August, CVS announced that Narcan would be available for purchase without a prescription – technically via a collaborative “blanket prescription” agreement with Dr. Rich – at 60 pharmacies, statewide. That same month, RI Dept. of Corrections Director A.T. Wall announced the DOC’s intent to begin distributing Narcan to prisoners upon release– a time when newly-released men and women are especially vulnerable to overdose, because their tolerances have dropped drastically since pre-incarceration usage. Jared Moffat and his wife, Rebecca McGoldrick, are already giving weekly overdose-prevention sessions, which include a Narcan 101 component, inside the prison’s walls.
“Before 2014, hardly anyone knew what Narcan was,” Michelle McKenzie says. “Now, many, many more people know.”
ARE THERE ANY SIDE EFFECTS?
Narcan/naloxone has virtually no side effects, Dr. Rich says. It won’t get you high, so there is no potential for abuse. And if a non-opioid user sprays it in their nose or injects themself, nothing much will happen.
Because it so effectively kicks the opiates out of the brain’s receptors, however, the medicine can put an opioid user into withdrawal.
”Many patients have described [withdrawal] to me as the most horrible feeling that you can imagine,” Dr. Rich says. “Imagine the worst flu you ever had in your life, and it’s ten times worse than that. People will do the most desperate and god-awful things to get out of withdrawal. And it’s something that really, unfortunately, drives a lot of people’s behaviors and drives this epidemic.”
As bad as withdrawal is, though, he says, it’s much better than letting someone die from an overdose.
GETTING STOCKED, GETTING TRAINED.
Narcan isn’t quite available for over-the-counter purchase in Rhode Island. But it’s close.
Thanks to Dr. Rich’s collaborative agreement, which Michelle McKenzie compares to the way pharmacists are allowed to administer flu shots, Rhode Islanders can walk into a CVS, a Rite-Aid, or a Walgreens and obtain a naloxone prescription.
“If you go to Walgreens,” McKenzie explains, “and you walk in, you go to the pharmacy and say, ‘I want naloxone.’ They’ll say, ‘OK. We need to get some information from you because Dr. Rich is going to be prescribing this medication to you.’ And they will take your insurance card, if you have it. And if you don’t they’re going to charge you $50 for two kits of intranasal or two kits of intramuscular naloxone, because they offer both. And then they do a brief, brief, brief little training about how to use it. And then off you go.”
Another option is dropping into PONI’s just-launched, free weekly Narcan trainings at AIDS Care Ocean State (ACOS), at 557 Broad Street, in Providence, on Tuesday nights. It took me about 25 minutes to be trained, when I stopped in on Opening Night, December 2. I watched a 13-minute YouTube video explaining how to recognize an overdose, and take the proper steps to respond to it. I filled out a quick questionnaire (“Are you currently using any opiates (including prescription opiates)?,” “Are you aware that using alcohol or pills like benzos (Klonipin, Xanax…) at the same time as opiates increase[s] your risk of fatal overdose?”). I took a short Narcan quiz. And I walked home with an orange plastic pill-canister containing two plastic-sealed syringes, two small glass vials containing doses of naloxone, and a cheat sheet with basic facts about the medication and responding to ODs.
I also got the chance to speak with Jonathan Goyer.
WHY NARCAN MATTERS
Jonathan Goyer remembers the date: June 16, 2013.
That was the day he overdosed on about $15 dollars worth of heroin while living in a recovery house in Pawtucket. Thankfully, the door to his room was left ajar and, when his roommate came home and spotted him, she ran downstairs to tell the house manager, who called 911 and ran upstairs with naloxone. When Goyer didn’t respond to the first injection, the house manager gave him another one. “My next conscious thought was when I was being brought out of the house on a stretcher going toward an ambulance,” Goyer says.
Goyer views those injections of Narcan as what saved his life.“If I didn’t get that second chance of life, to wake up in a hospital bed,” he says, “I woudn’t have been able to come to that realization that, ‘Holy sh**, I’m gonna die if I don’t get clean.’”
Eighteen months later, Goyer is a street outreach worker with the Providence-based nonprofit public health organization, Project Weber, and a volunteer with PONI. The 27-year-old is also RI’s resident Narcan celebrity, having been featured in the Rhode Island Medical Journal and the Providence Journal. In February, he told the paper, “My story is one that shows it’s worth saving lives.”
A FINAL NOTE
“No one is saying Narcan is the cure-all, by any stretch of the imagination,” says Dr. McDonald, from RIDOH. “But it does have that special niche role, which is to convert the overdose that would have been a death to just an overdose that’s now survived. Then you have that chance to have that conversation about, ‘What does treatment look like for this person?’”
Treatment is the best plan for someone struggling with the disease of substance abuse, McDonald says. But not everyone is ready.
“And for some of those folks, using this reversal agent is another way of keeping them alive for another day so we can keep the conversation going,” he says.
For more on naloxone, go to http://www.bhddh.ri.gov/misc/Narcan.php and http://prescribetoprevent.com.
 Phil Eil is the former News Editor for the Providence Phoenix. Eil grew up in Providence and is a Rhode Island Press Association Award recipient. He is a regular contributor to 630WPRO.COM.
Phil Eil is the former News Editor for the Providence Phoenix. Eil grew up in Providence and is a Rhode Island Press Association Award recipient. He is a regular contributor to 630WPRO.COM.
Follow him on Twitter (@phileil) and Facebook (facebook.com/phileilwriter), and email him at [email protected].